Closed on Memorial Day

Tuberculosis (TB) is a highly infectious disease that affects millions of people worldwide. To combat this global health concern, it is crucial to accurately diagnose and identify individuals at risk for TB. One common diagnostic tool used is TB skin testing. In this blog post, we will demystify the process and results of TB skin testing, providing you with a comprehensive understanding of its purpose, interpretation, and follow-up steps.
Before delving into TB skin testing, let’s first grasp the basics of tuberculosis. TB is caused by the bacterium Mycobacterium tuberculosis and primarily affects the lungs. It spreads through the air when an infected individual coughs or sneezes. TB remains a major public health challenge globally, with millions of new cases reported each year.
TB skin testing serves two primary purposes: identifying individuals at risk for TB and assessing latent TB infection. By identifying those at risk, healthcare providers can intervene early, preventing the development of active TB disease and reducing the transmission of the bacteria within communities. Furthermore, determining latent TB infection helps in implementing appropriate preventive measures and monitoring the health of individuals over time.
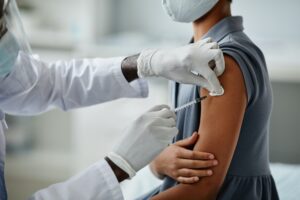
TB skin testing, often referred to as the Mantoux method, involves injecting a small amount of purified protein derivative (PPD) into the forearm. The test site is then evaluated for a delayed hypersensitivity reaction after a specific period. The procedure typically follows these steps:
The healthcare provider cleans the forearm using an antiseptic solution.
A small needle is used to inject a precise amount of PPD just below the skin's surface.
The provider marks the injection site to facilitate accurate reading.
The patient is advised to avoid touching or scratching the test site.
The patient is instructed to return within a specific timeframe (usually 48-72 hours) for a reading of the test site.
TB skin test results are based on the presence and size of induration, a raised and hardened area surrounding the test site. Interpretation guidelines for adults typically define positive results based on the induration size. However, the interpretation may differ for certain populations, such as children, elderly individuals, or those with weakened immune systems. Key points to consider when interpreting TB skin test results include:
A positive result indicates a delayed hypersensitivity reaction to the injected PPD, suggesting the presence of a TB infection. A negative result suggests the absence of a significant reaction and may indicate no TB infection or an inadequate immune response.
The induration size is measured and considered significant based on specific cutoff values. The cutoff varies depending on the population being tested and the risk factors involved.
Further diagnostic tests are often required to differentiate between latent TB infection and active TB disease. These tests may include chest X-rays, sputum cultures, or molecular tests.
Various factors, such as prior BCG vaccination, recent exposure to TB, or immunosuppressive conditions, can influence test results and should be taken into account during interpretation.
A positive TB skin test result necessitates further evaluation and follow-up steps to determine if active TB disease is present. Follow-up steps typically include:
Additional tests, such as chest X-rays and sputum cultures, are conducted to confirm the presence of active TB disease. Medical evaluation and treatment: Individuals with confirmed active TB disease require prompt medical evaluation and appropriate treatment regimens, typically involving a combination of antibiotics.
Contacts of individuals with active TB disease are identified and evaluated for TB infection. Those with latent TB infection may be offered preventive therapy to reduce the risk of progression to active TB disease.
Patients with TB, whether latent or active, should receive counseling on treatment adherence, infection control measures, and the importance of completing their prescribed regimen.
While TB skin testing is a valuable tool, there are certain challenges and considerations to keep in mind:
False-positive results may occur in individuals who have received BCG vaccination or have been exposed to non-tuberculosis mycobacteria. False-negative results can occur in individuals with weakened immune systems.
Prior BCG vaccination, recent exposure to TB, and immunocompromised conditions can impact the accuracy of TB skin testing and should be considered during interpretation.
TB skin testing cannot differentiate between latent TB infection and active TB disease. Additional tests are often necessary for an accurate diagnosis.
Healthcare workers, immigrants from high-prevalence areas, and individuals with HIV or other immunocompromised conditions may require specific considerations when interpreting TB skin test results.
To ensure the effectiveness and accuracy of TB skin testing, healthcare professionals should adhere to best practices, including:
Healthcare providers should be familiar with and adhere to national and international guidelines for TB screening and testing.
Proper infection control protocols, including the use of personal protective equipment, should be followed during the testing procedure.
Patients should receive clear instructions on the test procedure, follow-up steps, and infection control measures to minimize the spread of TB.
Efforts should be made to increase awareness, accessibility, and acceptance of TB skin testing, particularly among high-risk populations.
Ongoing research aims to improve TB screening and diagnosis. Promising developments include the introduction of new diagnostic tools, such as interferon-gamma release assays (IGRAs), which measure the immune response to TB-specific antigens. Additionally, researchers are exploring novel biomarkers and approaches that could revolutionize TB detection and management in the future.
TB skin testing plays a vital role in identifying individuals at risk for TB and assessing latent TB infection. Understanding the process and interpreting the results accurately is crucial for implementing appropriate preventive measures and ensuring prompt treatment when necessary. By following best practices, healthcare professionals can contribute to TB control efforts and reduce the burden of this global health concern. Through ongoing research and advancements in TB testing, we can look forward to improved screening and diagnosis methods that will further enhance our ability to combat this formidable disease.
Remember, if you have any concerns about TB or suspect you may have been exposed, it is essential to consult with a healthcare professional for proper evaluation and guidance. Together, we can work towards a future free from the burden of tuberculosis
Tuberculosis (TB) is a highly infectious disease caused by the bacterium Mycobacterium tuberculosis. It primarily affects the lungs but can also impact other parts of the body. TB spreads through the air when an infected individual coughs or sneezes.
The purpose of TB skin testing is to identify individuals at risk for TB and assess latent TB infection. It helps healthcare providers intervene early, prevent the development of active TB disease, and reduce transmission within communities.
TB skin testing involves injecting a small amount of purified protein derivative (PPD) just below the skin’s surface, usually in the forearm. The test site is then evaluated for a delayed hypersensitivity reaction after a specific period (usually 48-72 hours).
TB skin test results are based on the presence and size of induration, a raised and hardened area around the test site. Interpretation guidelines define positive results based on the induration size. However, the interpretation may vary for certain populations and risk factors.
A positive result suggests a delayed hypersensitivity reaction to the injected PPD, indicating the presence of a TB infection. Further diagnostic tests are usually required to differentiate between latent TB infection and active TB disease.
Yes, false-positive results can occur in individuals who have received BCG vaccination or have been exposed to non-tuberculosis mycobacteria. False-negative results can occur in individuals with weakened immune systems.
A positive result requires further evaluation to determine if active TB disease is present. Additional tests, such as chest X-rays and sputum cultures, are usually conducted to confirm the diagnosis. Prompt medical evaluation and treatment are necessary if active TB disease is detected.
TB skin testing cannot differentiate between latent TB infection and active TB disease. Additional tests are often necessary for an accurate diagnosis. Other factors, such as prior BCG vaccination or immunosuppressive conditions, can also impact test accuracy.